Yes! Risk of Stroke Can Be Drastically Reduced
By Eva Briggs, M.D.
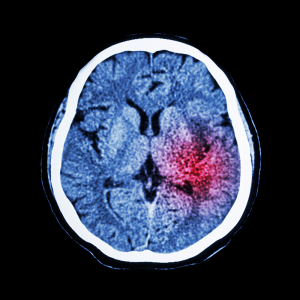
Every year about 800,00 people in the United States suffer strokes, making the disease the fifth-leading cause of death. Strokes involve blockage of blood flow to the brain, causing cells to die. It’s an emergency: a brain attack. There are two basic types of stroke. Hemorrhagic strokes, bleeding from the brain, cause about 15 percent of strokes. Ischemic strokes, the most common type of stroke, account for about 85 percent of strokes.
In this column I’ll talk about ways to reduce the chance of recurrence after a first ischemic stroke.
But first a recap of stroke symptoms and what to do if you think someone might be having a stroke. The following comes from the National Stroke Association, urging people to act FAST.
F-A-S-T
F: FACE:
Ask the person to smile. Does one side of the face droop?
A: ARMS:
Ask the person to raise both arms. Does one arm drift downward?
S: SPEECH
Ask the person to repeat a simple phrase. Is their speech slurred or strange?
T: TIME:
If you observe any of these signs, call 9-1-1 immediately.
That last item — time — is critical. Time is brain. If you see those symptoms call 9-1-1. Don’t stop at the urgent care or your doctor’s office first.
About one-half of patients who survive an ischemic stroke or TIA (sometimes called a mini stroke, a brief episode similar to a stroke that resolves on its own) are at risk for another stroke within days or weeks.
But modifying risk factors can reduce this chance.Here’s what you need to know.
Hypertension. This major risk factor can be treated in part with changes to lifestyle, such as weight loss, reduced salt intake, a Mediterranean-style diet, and regular aerobic physical activity. Patients whose blood pressure exceeds 140/90 may need blood pressure lowering medicine. For patients who don’t want to take medicine but have hypertension, it’s OK to start lifestyle changes and medication together, and wean off the medicine if the lifestyle measures are successful.
Diabetes. All patients with ischemic stroke should be tested for diabetes, and treated if present.
Hyperlipidemia. The American Heart Association and American College of Cardiology no longer recommend specific target levels for cholesterol. Instead, every patient with ischemic stroke due to atherosclerosis should take a statin regardless of cholesterol level.
Obstructive sleep apnea. About 50-75 percent of ischemic stroke patients have sleep apnea, often undiagnosed. So testing for sleep apnea is indicated for patients with ischemic stroke. Sleep apnea may cause symptoms such as daytime sleepiness, loud snoring, breathing interruptions or awakenings from gasping or choking.
Tobacco. Tobacco use is a risk factor for ischemic stroke, and just one more reason to quit smoking and avoid second-hand smoke.
Alcohol. Drinking more than two drinks per day or more than four drinks at a sitting increases ischemic stroke risk.
Exercise. Regular physical activity improves stroke risk factors such as diabetes and hypertension. The goal is at least 120 minutes per week of moderate to vigorous intensity exercise. Patients whose stroke symptoms make exercise difficult (weakness, balance impairment, altered thinking) may benefit from other physical activities.
Blood thinners. Antithrombotic medicine (drugs that reduce blood clot formation) often help reduce the risk of another ischemic stroke. These medicines include aspirin, clopidogrel, and dipyradamole, sometimes used in combination. The patient’s physician will individualize the preferred drug regimen.
Eva Briggs is a medical doctor who works at two urgent care centers (Central Square and Fulton) operated by Oswego Health.

